If your periods aren’t coming on time, you’re always tired, or you’re having trouble getting pregnant, your body may be trying to tell you something.
Endometriosis, thyroid, and PCOS are three conditions that rarely travel alone. Your hormones are closely connected, and when one is out of balance, the others often follow suit. Problems with ovulation, estrogen dominance, and chronic inflammation can all work together in the background to make it harder to get pregnant than it should be. Most people don’t know how important their thyroid really is. If your TSH levels are off, it can mess up your whole reproductive system, making a problem that seems small into something much bigger.
First, we need to understand how thyroid health is related to endometriosis and PCOS. Only then can we find real answers. There is no fancy language in this blog; it just tells you what you need to know in plain English.
- Get a free first consultation: Book an appointment.
- Call/W +91 9311850412 Email: info@fertilityworld.in
Why Are So Many Women Diagnosed With More Than One Hormonal Disorder?
You probably have PCOS, and then find out that your thyroid is also off. This doesn’t happen by accident very often. Your hormones work together, and when one is having a hard time, they all feel it. This is the main reason why most endocrine problems in women happen at the same time.
Is it a coincidence – or is there a deeper hormonal connection?
Not at all. There is a strong link between PCOS and thyroid problems. Both can affect insulin, inflammation, and reproductive hormones, and having one increases the likelihood of the other. Endometriosis has a similar pattern, and it often happens at the same time as autoimmune reactions, which are times when the body quietly fights itself.
All of this is linked by long-term inflammation. It stops ovulation, hurts the reproductive environment, and causes hormonal imbalances that make it hard to get pregnant for reasons that no one explanation can fully explain. That’s why pregnancy tests need to consider more than one factor. Because most of the time, the real answer is somewhere in the chain of them all.
Underlying Hormonal & Biological Mechanisms
| Condition | Primary Hormone Issue | Root Trigger | Inflammation Level | Autoimmune Risk |
|---|---|---|---|---|
| PCOS | Androgen excess | Insulin resistance | Moderate | Low |
| Endometriosis | Estrogen dominance | Immune dysfunction | High | Moderate |
| Thyroid Disorder | TSH imbalance | Autoimmune antibodies | Moderate | High |
What is PCOS and How Does It Affect Fertility?
PCOS (Polycystic Ovary Syndrome) is one of the most common hormonal problems in women and a major cause of pregnancy problems. At its core, it messes up the hormones that tell your body to release an egg every month. Not an egg, not a baby. The good news is that it’s not impossible to get pregnant, and many women with PCOS do.
Why Does PCOS Cause Irregular Ovulation?
Three things often go wrong at the same time in people with PCOS:
- Insulin resistance causes the ovaries to produce excess androgens, male hormones. This throws off your whole cycle.
- Then, too much androgen prevents follicles from developing properly, delaying or preventing the release of eggs. This is what causes most fertility problems in people with PCOS.
- Simply put, having irregular cycles with PCOS means that you probably don’t ovulate on time or at all, which makes it harder to get pregnant.
Can You Get Pregnant Naturally With PCOS?
Yes, and many people do. But some people do need a little help, and that’s fine. Often, the first step is to start ovulation by taking medicine like Letrozole or Clomid. This helps the body release eggs more regularly. PCOS and IVF are well-known routes with success rates for people who need more help. The important thing is to find the method that works best for your body, since PCOS and getting pregnant look different in each woman.
PCOS Fertility Treatment Options Compared
| Treatment | Best For | Success Rate |
|---|---|---|
| Lifestyle Changes | Mild PCOS, insulin resistance | Moderate improvement |
| Ovulation Induction (Letrozole/Clomid) | Irregular ovulation | 20–40% per cycle |
| IUI | Mild fertility issues | 10–20% per cycle |
| IVF | Severe PCOS, failed other treatments | 40–60% depending on age |
What is Endometriosis and Why Does It Reduce Fertility?
Endometriosis happens when tissue that looks like the lining of your uterus starts to grow outside of it. This tissue doesn’t have anywhere to go, so it’s not normal. This happens every month and makes it grow, bleed, and hurt. Over time, this makes conditions that really make getting pregnant hard. Lots of people go through this, and most don’t know how common it is.
How Does Endometriosis Affect Egg Quality?
It’s not always easy to see the damage that endometriosis does, but it’s real. What’s going on inside in the background:
- When you have chronic ovarian inflammation, it makes the area around your ovaries toxic, which lowers the quality of your eggs over time.
- When scar tissue forms around the fallopian tubes, it can block the egg’s path.
- When the lining of the uterus gets too swollen to hold a fertilised egg, the chances of implantation drop.
This is why endometriosis and impotence go hand in hand.
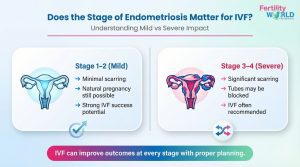
Does the Stage of Endometriosis Matter for IVF?
That’s true, but it’s not the whole story. It’s easy to understand:
- Stages 1 and 2 (Mild): Fewer scars, spontaneous conception is still possible, and IVF success rates are better.
- Stages 3 and 4 (Severe): More scarring, blocked tubes, and a lower chance of getting pregnant naturally. IVF is still a good choice.
Should you have surgery before IVF?
- Getting rid of lumps or scar tissue first can improve things.
- Sometimes, especially when the ovarian reserve is already low, it’s better to go straight to IVF.
What is Thyroid Disorder and Its Role in Fertility?
Most people don’t know how much power their small thyroid gland really has. It runs your whole body, from your digestion to your period. Your whole reproductive system feels the difference when it’s not working right. And it’s a shame that thyroid problems are often overlooked as a reason why women can’t get pregnant.
How Does Hypothyroidism Affect Ovulation?
TSH levels go up when your thyroid isn’t working as well as it should, and that’s where the trouble starts:
- Hormonal transmission is messed up by high TSH, which causes ovulation to happen irregularly or not at all.
- Periods become less regular, which makes it harder to get pregnant naturally.
- The lining of the uterus doesn’t form properly, which greatly raises the risk of failure during implantation.
Simply put, hypothyroidism and fertility don’t mix well – and many women don’t even know their thyroid is the missing piece.
Can Thyroid Imbalance Cause Miscarriage?
Yes, and more people should know this. Even a slightly off thyroid can affect early pregnancy. A lot of women who lose multiple pregnancies have autoimmune thyroid problems like Hashimoto’s thyroiditis. Usually, the best TSH values for getting pregnant are between 1.0 and 2.5 mIU/L, which are slightly higher than the normal range. Getting your thyroid levels in check before you try IVF or normal conception makes the chances of success much higher.
The good news? Thyroid problems that affect fertility can be easily managed with the right care and medicine.
PCOS vs Endometriosis vs Thyroid – Quick Comparison
| Condition | Hormonal Cause | Ovulation | Period Pattern | Fertility Risk |
|---|---|---|---|---|
| PCOS | Androgen excess, insulin resistance | Often irregular | Irregular | Delayed pregnancy |
| Endometriosis | Estrogen dominance, inflammation | Usually normal | Painful | Egg & implantation issues |
| Thyroid Disorder | TSH imbalance | Disrupted | Heavy/Irregular | Miscarriage risk |
Each condition affects fertility differently – but all three share one root: hormonal imbalance that needs attention, not guesswork.
What’s the Real Link Between PCOS, Endometriosis & Thyroid?
These three conditions which is PCOS, Endometriosis & Thyroid may seem unrelated – but underneath, they’re speaking the same language. That language is inflammation, estrogen, and immune dysfunction. Understanding how they connect is what changes everything.
Is Inflammation the Common Root Cause?
In a word, yes. A quiet thread of chronic inflammation links all three diseases. It stops the ovaries from working properly, messes up immune system signals, and prevents hormones from acting properly. A lot of women who have PCOS, endometriosis, or autoimmune thyroid problems have high levels of inflammatory markers. The thread is the main one that connects them.
Does Estrogen Dominance Connect Them?
Of course. When someone has endometriosis, too much estrogen causes tissue to grow outside of the uterus. In PCOS, an imbalance in hormones changes the amount of estrogen to progesterone, which stops ovulation. And when someone has a thyroid problem, estrogen dominance can make the thyroid work even less well. Androgen dominance and infertility go hand in hand. It appears differently in each problem, but the cause is usually the same.
Can Autoimmune Thyroid Trigger Reproductive Issues?
Yes, a lot more than most people think. Women who have endometriosis are more likely to have anti-TPO antibodies, which are a sign of autoimmune thyroid activity. Based on this overlap, the immune system isn’t just fighting the thyroid; it may also be affecting the reproductive environment. Now, doctors are paying a lot more attention to the link between autoimmune thyroid and pregnancy.
The Gut-Hormone Connection – Is Your Microbiome Affecting Fertility?
Your gut does far more than digest food. It quietly regulates your hormones – and when it’s out of balance, your reproductive health pays the price.
What is the Estrobolome?
The estrobolome is a group of gut bacteria that controls how estrogen is metabolized and recycled in your body. When gut health is poor, estrogen doesn’t get eliminated properly – it recirculates, builds up, and creates the kind of estrogen dominance that feeds endometriosis and disrupts fertility.
How Does Gut Health Affect Thyroid Function?
There are about 70% of your immune cells in your gut. It’s called “leaky gut” when the gut lining becomes permeable. This can trigger autoimmune reactions that directly impair thyroid function. Not getting enough of important nutrients like selenium, zinc, and iodine makes thyroid health even worse, and it’s hard to break the cycle without first fixing the gut.
Can Gut Inflammation Worsen PCOS Symptoms?
Yes. Insulin resistance is caused by gut inflammation. This inflammation makes chronic low-grade inflammation worse and makes the hormonal imbalance that makes PCOS harder to control even worse. Many women with PCOS feel a big difference in their symptoms when they take care of their gut health along with their regular treatment.
New study suggests that improving gut health may help women with PCOS, endometriosis, and thyroid disorders get their hormones in balance, especially when used with treatment that focuses on fertility.
Genetic & Environmental Triggers – What Might Be Increasing Your Risk?
Your risk of developing these conditions isn’t always random. Sometimes, it runs in the family — and sometimes, it’s the world around you quietly tipping the balance.
Is There a Genetic Predisposition?
You are more likely to get PCOS, endometriosis, or a thyroid problem if your mother or sister does. There is a lot of evidence that thyroid problems, PCOS, and endometriosis run in families. Genes don’t decide your fate, though; they’re only a part of it.
How Do Endocrine Disruptors Affect Hormones?
Xenoestrogens are chemicals that are found in everyday things, like microplastics, BPA in plastics, phthalates in makeup, and poisons in food. They work in the body like estrogen. They mess up the ovaries’ ability to function, the thyroid’s ability to send signals, and the inflammation’s ability to persist over time. EDCs and fertility are the subject of more study than ever before, and the results are hard to ignore.
Can Lifestyle Amplify Hormonal Imbalance?
Cortisol levels rise when you’re under a lot of stress, which lowers sexual hormones. If you don’t get enough sleep, your body’s hormones won’t work as they should. A diet high in processed foods makes inflammation worse, and not moving around much makes insulin resistance worse in people with PCOS. None of these things causes disease by itself, but when they come together, they create the perfect storm. Often, the environment, not genes, pulls the trigger.
Shared Symptoms – Why Diagnosis Gets Confusing
| Symptom | PCOS | Endometriosis | Thyroid |
|---|---|---|---|
| Irregular cycles | Yes | Sometimes | Yes |
| Severe period pain | No | Yes | No |
| Weight gain | Yes | Rarely | Yes |
| Fatigue | Yes | Yes | Yes |
| Hair thinning | Yes | No | Yes |
| Difficulty conceiving | Yes | Yes | Yes |
How Do These Conditions Together Impact Fertility?
Trouble with your thyroid, PCOS, or both can make it harder to get pregnant. Every condition changes a different part of the process of getting pregnant, making the journey longer and harder than it needs to be.
What Happens to Ovulation?
Ovulation is often delayed or not happening at all in women with PCOS because their hormones are out of whack due to too many androgens and insulin resistance. Another factor is an imbalanced thyroid, which can disrupt the hormonal signals your brain sends to your ovaries during each cycle. Because of this, the body has trouble releasing an egg regularly, making natural conception difficult to plan.
What Happens to Egg Quality?
Endometriosis causes toxic stress around the ovaries, which slowly lowers the quality of the eggs that are made. When thyroid chemicals are out of balance, the problem gets worse. Not only does a bad egg lower the chances of getting pregnant, but it also hurts the health of the developing baby in the early stages.
Why Does Implantation Fail?
Implantation can fail even after pregnancy. This is what’s going against it:
- A thin or inflamed endometrium, which can occur with thyroid problems and endometriosis, is not a good place for an embryo to settle.
- When the immune system is compromised, the body may sometimes reject a healthy baby for no clear reason.
- The lining of the uterus doesn’t thicken as it should each cycle because of hormonal problems.
Fertility Impact Breakdown
| Condition | Ovulation Impact | Egg Quality | Implantation | Miscarriage Risk |
|---|---|---|---|---|
| PCOS | Delayed | Mild impact | Possible | Slightly higher |
| Endometriosis | Normal ovulation | Often reduced | Reduced | Moderate |
| Hypothyroidism | Irregular | Reduced | Poor | Higher |
Can You Have PCOS, Thyroid & Endometriosis Together?
Yes, and more people don’t know about this than they think. A lot of people are treated for one illness for years while the others go unnoticed. This could be why you still feel “off” after getting a diagnosis.
How Common Is This Combination?
The link between PCOS and thyroid problems is one of the best-known in women’s hormonal health. Studies show that about 25 to 30 per cent of women with PCOS also have problems with their thyroids. Endometriosis and autoimmune thyroid disease are linked for the first time, but more and more studies show that immune system problems link them. These conditions don’t just live together; they make each other worse.
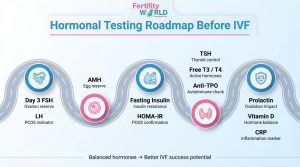
Why Full Hormonal Testing Is Essential Before IVF?
Going into IVF without knowing everything about hormones is like trying to put together a puzzle that is missing pieces. Before starting any fertility treatment, your doctor should look at:
- AMH: to find out how many eggs you have and how many of them you have left.
- TSH, T3, T4, and Anti-TPO: to rule out thyroid problems or inflammatory activity.
- Insulin and fasting glucose tests: These are used to determine whether PCOS is associated with insulin resistance.
- Inflammatory markers: to find out if long-term inflammation is quietly affecting your reproductive surroundings
This will save you time, money, and heartache if you do it right the first time.
Recommended Fertility Tests
| Condition | Important Tests | Ideal Fertility Range |
|---|---|---|
| PCOS | AMH, LH/FSH, Insulin | AMH moderate, LH/FSH balanced |
| Endometriosis | Ultrasound, MRI, CA-125 | Early detection is key |
| Thyroid | TSH, T3, T4, Anti-TPO | TSH 1.0–2.5 mIU/L |
The Psychological Impact – How Hormonal Disorders Affect Mental Health
It’s not just physical to live with PCOS, thyroid imbalance, or endometriosis. It’s also mental. A lot of women carry worry, mood swings, and the weight of not knowing what will happen for years. Taking care of mental health along with hormone therapy is not a choice; it’s a must for full fertility care.
Why Are Anxiety and Depression Common in PCOS?
PCOS and anxiety are linked in more ways than just stress. Neurotransmitter function can be directly affected by insulin resistance, which can change how your brain controls your mood. Higher amounts of androgen may make it even harder to keep your emotions in check, and visible symptoms like weight gain, acne, and hair growth that you don’t want can slowly destroy your confidence. It’s not a surprise that PCOS and sadness often go together. Hormonal problems can give you a lot of stress. Your body doesn’t hold on to the chemical chaos. You can also see it in your mind.
How Does Thyroid Imbalance Affect Emotional Stability?
Most people don’t know this, but your thyroid and mental health are linked. Everything slows down when you have hypothyroidism, even your mood. Hypothyroidism and sadness are both known to cause low energy, brain fog that won’t go away, and a heavy feeling that you can’t shake. Hyperthyroidism, on the other hand, speeds things up, which can cause worry, restlessness, and even panic-like symptoms. Both extremes change the amounts of serotonin, which makes it really hard to stay emotionally stable. A lot of women get help for years for mood problems before their thyroid is checked. That must change.
Does Stress Itself Worsen Fertility Outcomes?
In fact, this isn’t about “just relaxing.” When cortisol levels stay high for a long time, they mess up the hormonal signals needed for ovulation and the implantation window. Over time, this can cause mental burnout, which makes it harder for women to stick with their treatment. Mental health and getting pregnant go hand in hand. It’s not a matter of willpower, but biology that makes it less likely for a woman who is mentally drained to respond well to treatment
The Fertility Patient Roadmap — What Tests Should You Ask For?
If something feels off with your cycle, your energy, or your ability to conceive — don’t wait for someone to connect the dots for you. Ask for a complete hormonal panel. One test rarely tells the whole story.
If You Suspect PCOS, Thyroid Imbalance, or Endometriosis — Here’s What to Check
| Test | When to Do It | Why It Matters |
|---|---|---|
| Day 3 FSH | Cycle Day 2–3 | Measures ovarian reserve |
| LH | Cycle Day 2–3 | Elevated in PCOS |
| AMH | Any day | Egg reserve indicator |
| Fasting Insulin | Morning fasting | Detects insulin resistance |
| HOMA-IR | With insulin test | Confirms metabolic PCOS |
| TSH | Any time | Thyroid regulation |
| Free T3 & Free T4 | Any time | Active thyroid hormones |
| Anti-TPO Antibodies | Any time | Autoimmune thyroid detection |
| Prolactin | Morning | Can suppress ovulation |
| Vitamin D | Any time | Supports hormonal balance |
| CRP | Any time | Detects chronic inflammation |
Why Is Day 3 Testing Important?
Day 2 or 3 of your cycle is when hormones are at their most stable and readable. It gives your doctor the clearest picture of your ovarian function, catches PCOS patterns early, and provides an accurate baseline before any treatment begins.
What Is the Ideal TSH Level When Trying to Conceive?
This one shocks a lot of women. The normal TSH level is up to 4.5, but most fertility doctors say that when you’re trying to get pregnant, you should keep it between 1.0 and 2.5 mIU/L. Even more strict rules apply before IVF. On a standard report, a TSH level that seems “normal” might still be too high for a safe pregnancy.
Fertility Tip: If your periods are painful, your cycles aren’t regular, or you can’t get pregnant for no clear reason, get a full hormones panel, not just one test. If you only treat your thyroid or PCOS, you might not see the bigger picture.
Does Treating Thyroid Improve IVF Success?
Yes, and the study backs that up. Success rates are much higher when underlying hormonal problems are found and handled before IVF starts. You need to make sure that your hormones are in the best shape possible before you can get pregnant.
What Is the Ideal TSH Before IVF?
Before beginning an IVF treatment, most fertility doctors want to see a TSH level between 1.0 and 2.5 mIU/L. When thyroid levels are outside of this range, there is a much higher chance of an early miscarriage or failure of the embryo to implant. Thyroid imbalance is one of the easiest fertility problems to treat- a simple change in medication can bring levels back into the right range within weeks, making thyroid and IVF results much better.
Does Controlled PCOS Increase IVF Success?
Yes — when PCOS is well-managed before IVF, outcomes improve considerably. Women with PCOS typically produce more eggs during stimulation, which can actually work in their favour. The key is careful monitoring to avoid ovarian hyperstimulation syndrome (OHSS). With the right protocol and controlled insulin levels, IVF success rates in PCOS patients are genuinely encouraging – often comparable to women without the condition.
Can Endometriosis Patients Still Have High IVF Success?
They can – and many do. While endometriosis does affect egg quality and implantation, IVF bypasses many of the obstacles it creates naturally. Stage 1 and 2 patients often see strong results. Even with Stage 3 or 4, the right preparation – whether surgical or hormonal – significantly improves endometriosis IVF results. The journey may need more careful planning, but success is absolutely within reach.
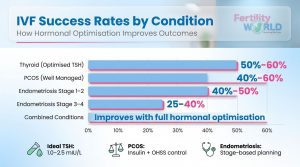
IVF Success Rate by Condition & Stage
| Condition | Approximate IVF Success Rate | Key Factor |
|---|---|---|
| Thyroid (Optimised TSH) | 50–60% | TSH controlled to 1–2.5 mIU/L |
| PCOS (Well Managed) | 40–60% | Insulin controlled, OHSS monitored |
| Endometriosis Stage 1–2 | 40–50% | Hormonal preparation |
| Endometriosis Stage 3–4 | 25–40% | Surgery or suppression first |
| Combined Conditions | Varies — improves significantly with full hormonal optimisation | Multi-targeted treatment approach |
Final Thoughts
We know how hard it is-all the meetings, questions that don’t get answered, and months of hope and wondering why things aren’t going as planned. If your periods aren’t regular, your periods hurt, or you’re having trouble getting pregnant, we want you to know that you are not alone and that you are not dreaming things.
There is a strong Link Between Endometriosis, Thyroid & PCOS problems. Once you understand that link, you can start to heal. You don’t need to keep putting things together by yourself. Everything can change if you see the right doctor, get the right tests, and follow a treatment plan that takes into account all of your hormones.
There’s nothing wrong with your body. It’s looking for the right kind of help. And you have every right to find it. We’re proud of you every step of the way.
Does PCOS always cause infertility?
No — many women with PCOS conceive naturally or with minimal medical support.
What is the ideal TSH level when trying to get pregnant?
Most fertility specialists recommend keeping TSH between 1.0–2.5 mIU/L for conception.
Can endometriosis affect egg quality?
Yes — chronic inflammation caused by endometriosis can gradually reduce egg quality over time.
Is thyroid imbalance linked to miscarriage?
Yes — uncontrolled thyroid levels, especially with autoimmune thyroid conditions, increase miscarriage risk.
Can lifestyle changes improve PCOS symptoms?
Yes — an anti-inflammatory diet and insulin regulation can significantly improve hormonal balance in PCOS.
Does stress worsen hormonal disorders?
Yes — chronic stress raises cortisol, which disrupts ovulation and deepens hormonal imbalance.
Is endometriosis genetic?
It can be — women with a close family member with endometriosis have a higher risk of developing it.
Can IVF work for women with endometriosis?
Yes — with the right preparation, IVF can be highly effective even in advanced endometriosis stages.
Should thyroid be treated before starting IVF?
Absolutely — optimising thyroid levels before IVF significantly improves implantation and success rates.