If you’ve been through one or more IUI cycles without a positive result, first – take a breath. You’re not alone, and this doesn’t mean your journey is over. It just means it might be time to ask a different question: How to know when it’s time to move from IUI to IVF?
It’s a decision many couples face, and honestly, it can feel overwhelming. But understanding the right moment to make this shift – from success rates by age to specific medical signs – can actually bring more clarity than confusion. Knowing how to know when it’s time to move from IUI to IVF helps you walk into your next conversation with your doctor feeling informed, not anxious. Let’s walk through it together.
- Get a free first consultation: Book an appointment.
- Call/W +91 9311850412 Email: info@fertilityworld.in
Understanding IUI vs IVF – What’s the Real Difference?
There are different types of fertility treatments, such as IUI and IVF. It is helpful to know what each one really involves, both physically and in terms of what your body goes through and your chances of getting pregnant. IUI, or intrauterine insemination, is a safer way to start. It’s easier on the body, costs less, and works well for mild pregnancy problems. In vitro fertilisation, or IVF, on the other hand, involves getting the eggs, fertilising them in a lab, and then transferring the baby.This is a more complicated process, but it has a much higher success rate per cycle.
Here’s a simple side-by-side of the difference between IUI and IVF:
| Factor | IUI | IVF |
|---|---|---|
| Procedure | Sperm placed in uterus | Egg retrieval + lab fertilization |
| Cost | Lower | Higher |
| Success Rate | 10–20% per cycle | 40–60% per cycle (age dependent) |
| Best For | Mild infertility | Moderate to severe infertility |
The IUI vs IVF success rate difference is significant – and for many couples, that gap becomes the deciding factor after multiple failed IUI attempts. Neither path is “better” in isolation; it all depends on your specific situation, your age, and what your fertility specialist recommends.
Has Modern At-Home Precision Tracking Improved IUI Success?
In the past few years, hormone tracking and ovulation monitoring tools that can be used at home have given couples a lot more control over time, which is very important for IUI. Tools that keep an eye on LH levels, body temperature, and even progesterone levels have made it easier for some couples to get the most out of their IUI treatments.
Better tracking can improve cycle time, but it doesn’t change the factors that really matter for success, like sperm quality, fallopian tube health, or egg reserve. Even if you’ve been very careful about tracking, if IUI still hasn’t worked, it’s probably not the time. There’s no need to worry if your body just needs a more direct method. It’s not failure, but knowledge.
How Many IUI Cycles Should You Try Before IVF?
Couples often want to know how many IUIs they should have before they should go for IVF. There is no one-size-fits-all answer, but most fertility doctors worldwide follow clear rules. If three IUI rounds fail, especially if the woman is over 35, most doctors will tell her to try IVF.
Age plays a significant role in this decision. Here’s what’s generally advised:
| Age Group | Recommended IUI Attempts Before IVF |
|---|---|
| Under 35 | 3–4 IUI cycles |
| 35–40 | 2–3 IUI cycles |
| Over 40 | Consider moving directly to IVF |
Ovarian reserve is the main reason why age is so important. The window for IUI to work narrows over time as egg quality and quantity naturally decrease. Also, waiting too long can lower the success rates of IVF. If you’re told you need IVF after a certain number of IUIs, it doesn’t mean something is wrong with you because your doctor wants to keep your chances high.
Why Age Changes the Equation Completely
If you’re over 35 and wondering how many IUI cycles you should do before switching to IVF at 35 or older? Not as many as you might think, to be honest. A good fertility expert will always look at your test results along with the amount of time that has passed. After age 35, the quality of eggs starts to drop more obviously. And each failed IUI cycle isn’t just a disappointment; it’s also time that could have been spent on a more likely method of conception. Because of this, a lot of doctors say that you should start IVF as soon as possible after that age.Giving IUI one more chance is not the same as giving up. Still, each couple’s path is unique.
Based on the diagnosis, some people move on to IVF sooner, while others wait to do all of the suggested cycles. The most important thing is that the choice is based on facts, not fear or fake hope.
5 Signs IUI Is Not Working and What to Do Next
Often, it’s not the treatment itself that’s hard; it’s not knowing when to change direction. If you’re still not sure if IUI is the right choice for you, your body and the results may already be telling you something significant. These are the main signs that IUI isn’t working and that you might need to talk to your doctor about what to do next.
Multiple Failed IUI Cycles
If you’ve tried 3–4 IUIs without getting pregnant, that trend is important to know. Not only is it upsetting, but it’s also important for medical reasons. After several failed rounds, the success rate of IVF is much higher, and this is when most doctors will start talking about switching. Continuing IUI past this point doesn’t usually make things better and might just delay a better answer.
Age Over 35
Age is one of the most honest ways to tell if someone is fertile. The success rate of IUI drops sharply after age 35, and the difference between IUI and IVF results gets bigger every year. If you’re in this age range and IUI hasn’t worked yet, you should start IVF as soon as possible to give your eggs and your chances the best chance of succeeding.
Low AMH or Diminished Ovarian Reserve
If your AMH levels are low or your reproductive tests show that your ovarian reserve has been reduced, IUI may not be able to help you. IVF, on the other hand, lets your doctor closely watch your eggs, pick out the best ones, and choose the healthiest embryos for transfer, which isn’t possible with IUI. This level of accuracy can make all the difference for women with few eggs left.
Male Factor Infertility
If there aren’t enough sperm, they might not move well, or their shape might not be right. IUI might not be able to help. IVF plus ICSI (Intracytoplasmic Sperm Injection), in which a single healthy sperm is injected straight into the egg, greatly raises the chances of fertilisation. It takes the guessing out of a process that is mostly up to chance with IUI.
Endometriosis or PCOS Complications
There are two diseases that can make IUI work much less well are Endometriosis and PCOS. Endometriosis can make it hard for sperm to move and eggs to be healthy in ways that IUI can’t fix. And while IUI can sometimes help with PCOS, IVF’s controlled stimulation and tracking is often much better for more complicated cases. If either of these is part of your diagnosis, IVF may just be the best way for you to get pregnant.
At a Glance: When to Stop IUI and Move to IVF
| Sign | Why It Matters | Recommended Next Step | |
|---|---|---|---|
| 1 | Multiple Failed IUI Cycles | After 3–4 failed attempts, continuing IUI rarely improves outcomes | Consider moving to IVF for significantly higher success rates |
| 2 | Age Over 35 | IUI success rates decline sharply after 35; every cycle counts | Move to IVF sooner to protect egg quality and chances |
| 3 | Low AMH or Diminished Ovarian Reserve | IUI cannot monitor or select embryos with low egg reserve | IVF allows precise egg monitoring and embryo selection |
| 4 | Male Factor Infertility | Low sperm count or motility limits IUI effectiveness | IVF with ICSI directly injects healthy sperm into the egg |
| 5 | Endometriosis or PCOS Complications | Both conditions can interfere with IUI in ways it cannot overcome | IVF’s controlled stimulation responds better to these conditions |
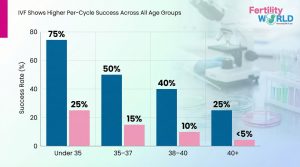
IUI vs IVF Success Rate by Age
If you’ve ever thought if IVF or IUI works better, the numbers make it clear. When you look at the success rates of IUI and IVF by age, you can see a pattern: as you get older, the difference between the two methods gets much bigger. And IVF has almost three times the success rate per session for younger women as well.
Here’s what modern data tells us:
| Age Group | IUI Success Rate (Per Cycle) | IVF Success Rate (Per Cycle) |
|---|---|---|
| Under 35 | 15–25% | 50–75% |
| 35–37 | 10–15% | 40–50% |
| 38–40 | 8–10% | 30–40% |
| 40+ | <5% | 15–25% |
It’s hard to miss the point: IVF gives people of almost every age a much better chance of getting pregnant each time. Success rates of IVF for women under 35 are now between 50 and 75% per cycle, which is even higher than the old standards because of improvements in genetic screening (PGT-A).
It’s also important to note that IUI success rates have slightly gone up. For younger women, the per-cycle rates have gone up to 15–25% thanks to better ways to clean sperm and track hormones. But there is still a significant difference between them, and it grows with age.
Why the Age Gap Matters More Than Most Couples Realise
While IUI can help you, it works better the younger you are. IUI success drops below 5% per cycle for women aged 40 and up. This means that there are very few chances of success each month. Even at that age, IVF still works 15–25% of the time, which makes it three to five times more effective. For couples in this age range, every cycle really does matter, and starting down the path to more success earlier can make all the difference.
Should You Try Another IUI or Move to IVF?
If you’re thinking about this question right now, know that you’re in one of the most human parts of the fertility journey. This is the point where hope, tiredness, money, and medical reality all come together. There’s no single right answer, but there are clear things that can help you choose between IVF and IUI again. Getting IVF doesn’t mean you’ve failed. It means picking a better way to treat the problem.
The 4 Factors That Should Guide Your IUI vs IVF Decision
- Emotional Exhaustion : Every failed IUI cycle is very hard on the emotions. That’s important to know if it’s getting harder to improve between rounds or if hope is fading faster than it used to. Your mental and emotional health is not separate from your road to get pregnant; it is part of it. Going with IVF isn’t always better for your health; sometimes it’s also better for your feelings.
- Financial Planning : IUI is cheaper per cycle, but the costs add up if you try more than once. IVF costs more up front, but many couples find that it is worth it in the long run because it has a much higher success rate per treatment. If you have already spent money on 3–4 rounds of IUI that didn’t work, the financial case for IVF usually gets better with each try.
-
Factor IUI IVF Cost Per Cycle Lower Higher Success Rate Per Cycle 15–25% 50–75% Total Cycles Typically Needed 3–4 1–2 Long-Term Cost Efficiency Lower Higher - Time Sensitivity : If you’re over 35, time is one of the most valuable things you can use to get pregnant. Every cycle spent on a treatment that doesn’t work as well as others is a cycle that could have been used on a treatment that did work better. When making this decision, your doctor will always take your age into account. You should pay close attention to why they’re pushing you towards IVF.
- Medical Diagnosis: If you have low AMH, male factor infertility, endometriosis, or tubes that are blocked, it is highly unlikely that IUI will work, no matter how many cycles you try. If any of these test findings apply to you, it’s not too early to switch to IVF from IUI. It means making the best choice you can with the knowledge you have.
Cost Comparison – Is IVF Worth It After Failed IUI?
One of the most practical questions couples ask is: Is IVF worth the cost after multiple failed IUI cycles? It’s a completely valid question – and when you look at the numbers honestly, the answer might surprise you.
IUI is more affordable per cycle, no question. But here’s what many couples don’t realise until they’re several cycles in – the cumulative cost of multiple failed IUIs can quietly creep up to match, or even exceed, the cost of a single IVF cycle. And all of that spending comes with a significantly lower chance of success.
Here’s a global cost comparison:
| Treatment | Cost Per Cycle (Approx.) | Success Rate Per Cycle | Average Cycles Needed | Estimated Total Cost |
|---|---|---|---|---|
| IUI | $300–$900 | 15–25% | 3–4 cycles | $900–$3,600 |
| IVF (Standard) | $8,000–$15,000 | 50–75% | 1–2 cycles | $8,000–$30,000 |
| IVF (India) | $2,500–$4,500 | 50–70% | 1–2 cycles | $2,500–$9,000 |
| Natural Cycle IVF | $1,500–$4,000 | 15–20% | 2–3 cycles | $3,000–$12,000 |
Costs vary by clinic, location, medications, and individual treatment protocols.
If you think about it this way, three to four failed IUI rounds costing $900 each add up to $2,700 to $3,600, and the success rate is still much lower than a single IVF cycle. When couples in India or other low-cost places are compared to repeated IUI tries, IVF becomes an even more appealing choice.
The Global Shift – Why More Couples Are Choosing IVF Sooner
There is a growing trend in fertility clinics around the world: couples are switching from IUI to IVF earlier in their journey. This isn’t because IUI isn’t useful; time and mental energy are also resources.It’s not only medically smarter to start IVF sooner, but it’s also financially and emotionally smarter in the long run. This is because of the months spent on each IUI cycle, the time it takes to recover emotionally between failed attempts, and the missed chance to start a more successful treatment.
The real question isn’t “Can we pay for IVF?” For many couples, the real question is: Can we afford to wait any longer?
If you’ve already tried multiple IUI cycles without success, one of the most empowering things you can do right now is talk to your specialist about how much IVF costs, how you can pay for it, and the chances of success that are specific to your case.
When Doctors Recommend Skipping IUI and Going Directly to IVF
Doctors will often do anything to save you time. Skipping IUI altogether isn’t giving up on a step in some medical situations; it’s just picking the right place to begin your trip.
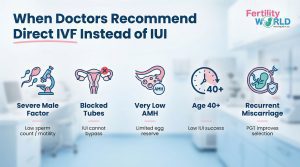
When doctors usually say to go straight to IVF, are these situations:
- Severe Male Factor Infertility: IUI can’t work when there aren’t enough sperm, or they can’t move around efficiently. Using ICSI in IVF lets doctors choose the best sperm directly, which increases the chances of fertilisation.
- Blocked Fallopian Tubes: To do its job, IUI needs open tubes. Infertility treatments (IVF) often remove them completely from the picture if they’re stopped.
- Very Low AMH: Every egg counts because the egg supply is limited. Experts can carefully collect and test those eggs during IVF, but not during IUI.
- Age 40 and above: Now, less than 5% of IUI cycles succeed. Shortcutting to IVF will save you time and improve your chances.
- Repeated Miscarriages: Using genetic screening (PGT-A) along with IVF can help find healthy eggs before they are transferred, lowering the chance of losing another baby.
If your doctor is recommending you skip IUI, they’re not closing a door — they’re opening the right one sooner.
What If You’re Not Sure Which Category You Fall Into?
This takes place more often than you think. It’s not always easy to tell what’s wrong, and not every pair has a clear medical reason to skip IUI. If you’re in the middle-with a weak male factor, borderline AMH, or infertility that can’t be explained-the choice is more complicated. That’s exactly why it’s important to get a full pregnancy checkup before making any decisions. An honest talk with your expert, blood tests, and an ultrasound can help you to understand when should you switch from IUI to IVF.
Your Next Step Doesn’t Have to Feel Scary
It’s not about giving up when you decide to switch from IUI to IVF. It’s about picking a better way to reach your goal. After several rounds of IUI that didn’t work, you may find that IVF works better, gives you answers faster, and makes a plan that is specifically tailored to your needs.You don’t need to do this by yourself.
At Fertility World, we put you in touch with experienced IVF doctors in India and around the world. These doctors will look at your whole situation before telling you what to do next. Don’t guess. You’ve found the right person. Send us a message right now, and we’ll help you find the doctor who can help you bring your baby home.
Is IVF more successful than IUI?
Yes. IVF offers 50–75% success per cycle for women under 35, compared to 15–25% with IUI. The gap only grows with age.
What are the main signs that IUI is not working?
Multiple failed cycles, age over 35, low AMH, male factor infertility, and conditions like endometriosis or PCOS are the most common signs.
Can I skip IUI and go directly to IVF?
Yes. Blocked tubes, severe male factor infertility, very low AMH, or repeated miscarriages are all cases where doctors often recommend starting directly with IVF.
Does moving to IVF mean IUI has failed completely?
Not at all. It simply means your situation needs a stronger approach. Moving to IVF is a step forward — not a sign that something went wrong.
How does age affect the decision to move from IUI to IVF?
After 35, IUI success drops sharply. Over 40, it falls below 5% per cycle. The older you are, the stronger the case for moving to IVF sooner.
Is IVF worth the higher cost after multiple failed IUIs?
Often yes. Multiple failed IUI cycles can cost as much as one IVF cycle — with far lower chances of success. IVF is frequently more cost-effective over time.
Can low AMH levels affect my decision between IUI and IVF?
Yes. Low AMH reduces IUI's effectiveness significantly. IVF allows careful egg retrieval and embryo screening — something IUI simply can't offer.
What is natural cycle IVF and is it a middle ground between IUI and IVF?
Natural cycle IVF uses your body's naturally produced egg — no heavy stimulation. It's gentler and more affordable, and can be a good bridge for younger women not ready for full IVF.
How do I know if my doctor is recommending IVF too soon?
Ask them to explain the specific medical reasons. A good specialist will always base the recommendation on your test results, age, and cycle history — never just cost.