Every IVF journey starts with hope, but at some point, a quiet, heavy question comes up: how many IVF cycles are safe, and when is enough, enough? You are not the only one who is asking this. A lot of women who are trying to get pregnant through IVF ask the same thing, usually after a failed cycle, a hard talk with their doctor, or a night of little sleep.
The honest truth is that there isn’t a single number. There is no one-size-fits-all answer to how many times can you do IVF safely. It depends on your age, your physiology, your diagnosis, and how you feel emotionally.
It is also true that IVF does not guarantee conception which is more important to know how many IVF cycles until pregnancy than any general number. This book talks about everything, from medical guidelines to the most important things to consider, age-based safety, and what to do next if IVF doesn’t work.
- Book an online appointment: Get a free fertility consultation.
- CallW: 9311850412
- Email: info@fertilityworld.in
What Doctors Actually Say About the Safe Number of IVF Cycles
Most people expect a clear number when they ask about the safe number of IVF cycles recommended by doctors. The truth is that there isn’t one. And knowing why that is actually helps you.
Medical Guidelines From Around the World
There are Medical guidelines for IVF cycle limits, but these are just starting points, not stop signs.
- NICE (UK) says that women under 40 who meet certain criteria should be able to get up to three full IVF cycles on the NHS. This is a recommendation for how to get money, not a safety decision. Women can and do continue privately after three cycles.
- ASRM (USA) does things quite differently; there is no set upper limit. Every choice is based on evidence, is made to the person in front of the doctor, and is made with that person in mind.
- ICMR (India) says that women should carefully think about each cycle and that there is no limit on how many IVF cycles are safe for a woman. The focus is on continuing review, not a hard stop.
The main point? These bodies are signalling when to take a break and think about their IVF cycle limit for women, not when to give up.
Why There Is No Maximum Number of IVF Cycles for One Woman
It’s worth thinking about that the maximum IVF cycles for one woman is not written in any global medical rulebook. There is no gap in medical knowledge; it is planned. Your body, your diagnosis, and your emotional condition all play a role in how many IVF cycles are too many. Some women have gotten pregnant on cycles 7 or 8. It’s not common, but it’s also not impossible.
You and your doctor should talk about how many IVF cycles are safe that you can have, not just look at a chart. Doctors do know this: safety is only one part of the puzzle. Clinically recognised as a factor is emotional exhaustion. Money problems are a real medical issue. Both are genuine, both are true, and both should be given an honest place in your treatment plan. Not having a definite limit doesn’t mean uncertainty; it means personalised medication is working as it should.
Factors That Determine How Many IVF Cycles You Need
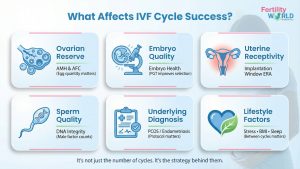
You did everything perfectly. You have kept every appointment, gotten every shot on schedule, and followed every instruction. But here you are again, after another failed cycle, asking the same painful question: why is this not working? You’re not the only one who feels bewildered, frustrated, and unsure of what’s really going wrong. The good news is that there is an answer. These are the things that really affect how many IVF cycles you may need and what could be silently getting in the way:
- Ovarian Reserve (AFC and AMH): Your eggs. Low AMH indicates fewer eggs per retrieval. Low AMH IVF cycles often necessitate a kinder, smarter approach. Tested before each new cycle.
- Embryo Quality: Not every embryo attaches. PGT-A genetic testing looks for chromosomal problems before the transfer, which directly affects the IVF success rate per transfer. Quality is always better than quantity.
- Uterine Health and Receptivity: A perfect embryo will not implant in a uterus that is not ready. ERA testing in IVF finds your exact implantation window. Fibroids, polyps, and adhesions quietly lower the chances of success over several cycles.
- Sperm Quality and DNA Fragmentation: The male component accounts for 40–50% of all reproductive issues, and it is frequently examined last. Even if a basic semen analysis appears normal, sperm DNA fragmentation can reduce the quality of an embryo.
- Diagnosis Underlying: PCOS, more eggs, but a higher risk of OHSS; managing the protocol is key. Endometriosis IVF cycles impair egg quality and uterine receptivity; may need surgical review. IVF for unexplained infertility, such as thyroid, immunological, and coagulation factors, is often not found until cycle 3 or later.
- Lifestyle factors: BMI, smoking, chronic stress, sleep, and diet all have a direct impact on egg quality and implantation. It’s not simply the shots that affect your health when you have several IVF rounds; what you do between cycles is just as important.
Key Factors and Their Impact on IVF Cycle Outcomes
| Factor | Impact Level | What to Test | When to Address |
|---|---|---|---|
| Ovarian Reserve (AMH/AFC) | Very High | AMH blood test + AFC ultrasound | Before every new cycle |
| Embryo Quality (PGT-A) | Very High | Blastocyst grading + genetic screen | Each retrieval cycle |
| Uterine Receptivity (ERA) | High | ERA test + hysteroscopy | After 2–3 failed transfers |
| Sperm DNA Fragmentation | High | DNA fragmentation index (DFI) | After 2 failed cycles |
| BMI and Lifestyle | Moderate–High | BMI + metabolic panel | Before starting IVF |
| Thyroid Function | Moderate | TSH, T3, T4 | Before and during IVF |
| Immune / Clotting Disorders | Moderate | ANA, NK cells, thrombophilia | After recurrent failure |
| Underlying Diagnosis | High | Full fertility workup | Ongoing reassessment |
Pregnancy Odds Per IVF Cycle – What the Numbers Say
When you’re dealing with something this personal, numbers can seem cold. But sometimes, genuine data is what gives us hope and makes things clear. This is what the numbers really indicate about how many IVF cycles until pregnancy and how likely you are to get pregnant with each one.
How Many IVF Cycles Does It Take to Conceive?
The truth is that most women who have successful IVF do so within three cycles. But that’s not where the narrative stops. The average number of IVF cycles needed to get pregnant goes up over time, so your odds don’t start over after a failed effort; they add up:
- Most successful pregnancies happen within the first 3 cycles
- IVF cycles needed to get pregnant can extend to 4–6, with success rates still climbing meaningfully
- After cycle 6, success rates begin to plateau for most patient profiles
- Crucially, every failed cycle is not a dead end. It is data. Each attempt tells your doctor something new about your body that can make the next cycle smarter’
How many IVF rounds are safe is one question, but how each round improves your odds when approached correctly is an equally important one.
Why Cycle 3 Is Not Your Last Chance
This is the overall IVF success rate by cycle number. Not only is it feasible for IVF success after repeated cycles, but the numbers show it:
Cumulative IVF Success Rate by Cycle Number
| IVF Cycle | Per-Cycle Success Rate | Cumulative Success Rate | Notes |
|---|---|---|---|
| Cycle 1 | 30–40% | 30–40% | Baseline attempt |
| Cycle 2 | 25–35% | 50–60% | Protocol adjustments help |
| Cycle 3 | 20–30% | 65–75% | Standard evaluation point |
| Cycle 4 | 15–25% | 72–80% | Deeper diagnostics recommended |
| Cycle 5 | 10–20% | 78–85% | Specialist review advised |
| Cycle 6 | 8–15% | 80–88% | Comprehensive reassessment |
Rates vary based on the patient’s age, diagnosis, clinic rules, and embryo quality. The numbers are averages from peer-reviewed research.
Why One Failed Attempt Is Not the Final Verdict
This is perhaps the most crucial thing to know about the first cycle IVF success probability: one failed effort doesn’t tell you much about your total prospects. The IVF failure percentage rate in cycle 1 can be as high as 60–70%, which is entirely normal. It doesn’t mean that IVF won’t work for you. This is why:
- Does IVF guarantee pregnancy? No, not at cycle 1 or any other cycle. But accumulated chances paint a much more positive narrative.
- If you fail in cycle 1, your clinic will learn important things about how your body responds to stimulation, the quality of your embryos, and how your uterus behaves.
- When doctors use data from the first IVF cycle to refine the protocol, the second IVF cycle outcome rates always increase.
- Most clinics make meaningful adjustments to medication doses, trigger timing, and transfer strategy after a first failed attempt.
A cycle that doesn’t work out isn’t the end of the narrative. For most women, it’s actually the start of a much better-informed one.
Does Age Affect How Many IVF Cycles Are Safe?
Age is one of the most honest things to talk about when it comes to fertility. It doesn’t determine your outcome, but it does impact your strategy. Here is what happens at each stage and how it affects the IVF success statistics by age group.
Under 35 – The Strongest Starting Point
If you’re under 35, good news: your ovarian reserve is at its highest point, and your reaction to stimulation is the most predictable it will ever be.
- Most women in this group can safely have up to six cycles.
- Higher in vitro fertilisation success odds by age mean fewer cycles are usually needed overall.
- The goal here is to optimize, not to haste.
After 35 – What Starts to Shift
IVF safety after 35 doesn’t mean IVF stops functioning; it means you need to change how you do things.
- Ovarian reserve starts to drop in a measured way: FSH goes up, and AMH goes down.
- The response to stimulation becomes less predictable over time.
- Second IVF cycle outcomes can still be good, but it’s more crucial to change the protocol.
- The talk of donating eggs usually comes up around 39–40 after failed attempts.
Over 40 – Realistic Odds and Smarter Decisions
This is when being honest is most important. IVF safety after 40 isn’t about whether it’s physiologically possible; it’s about making sure every cycle counts.
- How many IVF cycles are safe over 40? Most experts say you should try 3 to 4 times with your own eggs before considering other options.
- Success per cycle drops to 10–15% with own eggs– IVF at 43, with own eggs, the success rate is even lower at 5-10%
- Chromosomal problems get much worse as you get older. PGT-A testing is highly recommended for everyone over 38.
- Donor eggs increase the chances of success to 50–65% each transfer. This conversation should happen early on, not as a last resort.
IVF Success Rate and Recommended Cycles by Age Group
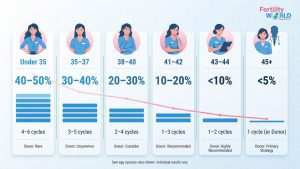
| Age Group | Success Rate Per Cycle (Own Eggs) | Recommended Cycles | When to Discuss Donor Eggs |
|---|---|---|---|
| Under 35 | 40–50% | 4–6 cycles | Rarely needed |
| 35–37 | 30–40% | 3–5 cycles | After 4–5 failed cycles |
| 38–40 | 20–30% | 3–4 cycles | After 3–4 failed cycles |
| 41–42 | 13–18% | 2–3 cycles | Discussed proactively |
| 43–44 | 5–10% | 1–3 cycles | Strongly recommended |
| 45+ | Less than 5% | 1–2 cycles | Usually the primary option |
When to Stop IVF – Knowing When It Is Time to Reassess
This is the hardest question in the IVF trying to conceive journey, but it’s also one of the most crucial. Stopping doesn’t mean quitting. It means being honest with yourself, your body, and your future. This is how to tell when that time has come. Sometimes the signal comes from the medical side first. These are the physical indicators that specialists look for when discussing how many IVF cycles before stopping:
- Consistent poor embryo quality across multiple stimulation cycles – this is a pattern, not just one time.
- Recurrent implantation failure with chromosomally normal embryos – When excellent embryos keep failing to implant, the research needs to go deeper.
- Significant decline in ovarian reserve with each cycle – fewer eggs, fewer embryos, and less return on investment.
- Physical symptoms – exhaustion, hormonal imbalance, or medical complications – that require genuine rest between cycles.
- When the risks of multiple IVF cycles begin to outweigh the realistic probability of success.
If your doctor sees these tendencies, talking about taking a break is not being negative; it is being responsible.
Emotional Signs – Feelings That Are Just as Valid as Test Results
It’s not just a medical question of how many IVF cycles are too many. Your mental wellness is as important as your physical health, and these indications should be treated the same way as any blood test:
- Long-term anxiety or clinical depression that is directly related to therapy, not just melancholy that comes and goes, but the impact of multiple IVF cycles on mental health.
- Relationship problems that have gone from stress to something worse
- Financially unsustainable indicates that if you keep going, your stability and security will be hurt for good.
- Loss of identity: when the IVF health journey starts to take over your life outside of the treatment rooms
You can remark, “This is having an effect on my life that I can’t handle anymore.” That isn’t being weak. That is being conscious of yourself, and that is very important.
Life After Repeated IVF Failures: Your Options Are Not Over
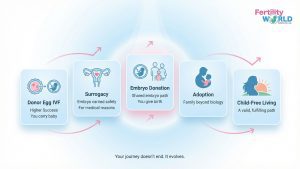
If IVF hasn’t worked for you, even after several tries, please know that you can still become a parent. It has just gone in a different direction. There are real, meaningful, and deeply fulfilling options after multiple IVF failures that thousands of families have walked before you. Here is what is available, explained honestly.
Donor Egg IVF – The Most Taken Step After Own-Egg IVF Fails
When your own eggs are the problem, donor egg IVF after failed cycles is the most typical and successful next step.
- A healthy donor who has been screened gives you the eggs, which are then fertilised with your partner’s sperm.
- You carry the baby and give birth, thus you are still a mother.
- Success rates jump to 50–65% per transfer, regardless of your age.
- The success rate for IVF at 43 with your own eggs is only 5–10%, but donor eggs make a big difference.
Best for: low AMH, being 40 or older, having bad embryos over and over again, or having genetic disorders. A lot of women say that donor egg IVF wasn’t giving something up; it was the choice that finally brought their baby home.
Gestational Surrogacy – When the Uterus Is the Barrier
If your embryos are healthy but implantation keeps failing, surrogacy after IVF failure may be the answer.
- A gestational surrogate carries your own embryo or a donor embryo.
- Recommended when uterine conditions are connected to recurrent implantation failure.
- Also appropriate when pregnancy poses a serious health risk to the mother
- The Surrogacy (Regulation) Act 2021 in India allows only altruistic surrogacy. Laws vary from country to country; it’s important to get legal advice before moving forward.
Best for: problems with the uterus, severe RIF, serious health problems, or numerous failed transfers with viable embryos.
Embryo Donation – A Quietly Powerful Option
Not talked about much, but very important. Embryo adoption after IVF failure involves getting a completely donated embryo from another couple’s IVF adventure.
- You carry the baby and give birth, but both partners aren’t genetically related to the baby.
- Success rates of 40-60% per transfer – comparable to donor egg IVF
- A more affordable alternative to fresh donor egg cycles
- Unused frozen embryos donated with full legal consent
Best for: couples where both egg and sperm quality are barriers, single women, same-sex couples. Many families who choose this path describe it as one of the most profound decisions they ever made.
Adoption – Building a Family Beyond Biology
Adopting after IVF failure is not a consolation prize; for many families, it is the happiest time of their lives.
- Following the rules set by CARA (Central Adoption Resource Authority) in India
- Includes home studies, background checks, and a period of waiting
- A way that is more likely to lead to a child than any IVF cycle
- It is strongly suggested that you get counselling support when you stop fertility therapy.
- Best for: people who feel that they should provide a child already in the world a caring home
Child-Free Living – A Brave and Valid Choice
It’s okay if not every narrative ends with a child. Living without children after infertility is a brave, well-thought-out choice, not a failure.
- It’s a real process of emotional healing after failed IVF, and it needs real help.
- Fertility counsellors who focus on finishing treatment might help you deal with your feelings and move on.
- Online groups for living child-free after infertility let them connect and understand each other.
- Redefining purpose, identity, and joy outside of parenthood is a path thousands have walked with fulfilment.
Which Alternative Should You Explore Next?
| Your Situation | Best Next Step |
|---|---|
| Good uterus, poor egg quality, age 40+ | Donor Egg IVF |
| Good embryos, failed implantation repeatedly | Gestational Surrogacy + ERA Investigation |
| Both egg and sperm quality are barriers | Embryo Donation |
| Completed clinical journey, open to all paths | Adoption or Child-Free Living |
| Still in treatment, high stress levels | Complementary Therapy + Counselling |
| Unexplained failure, no diagnosis found | Second Opinion + Deeper Diagnostics First |
Physical and Emotional Risks of Multiple IVF Cycles
Every time you go through IVF, your body and mind have to do something. One cycle is doable. But the more attempts you make, the more dangerous they become. Knowing the risks of multiple IVF cycles is not meant to terrify you; it’s designed to help you make better, safer choices at every step.
What Repeated IVF Stimulation Does to Your Body
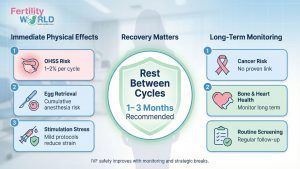
The physical effects of repeated IVF are real, but they can be managed if they are watched closely. OHSS risk is 1–2% moderate-to-severe per cycle, and it can be managed with low stimulation procedures. There is no confirmed long-term cancer link, although regular checkups are always a good idea.
Here are a few crucial things to remember:
- How many egg retrieval procedures are safe? Each has minimal but cumulative anaesthesia risks that are considered before each retrieval.
- Mild stimulation techniques greatly lessen the physical stress for those at high risk.
- The recommended time between stimulation cycles for recovery is 1–3 months. This is therapeutic advice, not a choice.
Long-Term Effects of IVF on Women
The honest answer is comforting, but it comes with a warning. So far, studies have not found that normal IVF therapy raises the risk of breast, ovarian, or endometrial cancer. But researchers are still looking into the safety of repeated IVF cycles over a long period of time.
- During long-term treatment, bone density and heart health should be monitored.
- It is also suggested to get regular health screenings between cycles.
- Breaks between cycles give the body a chance to heal in a measurable and meaningful way.
Conclusion: Your IVF Journey – Every Step Forward Counts
There is no one number of IVF cycles that is best for all women. Your body, age, diagnosis, and anything else that comes up along the way form your trip. It’s important to make the proper choice about alternatives after failed IVF. It takes guts to keep going. Knowing when to stop is also important. Both are correct and courageous.
And if IVF hasn’t worked yet, don’t forget that options like donor eggs, surrogacy, and adoption are not consolation prizes after unsuccessful IVF cycles. They are real, caring, and gratifying ways to get the family you want. You deserve personalised help, not just basic numbers, no matter what cycle you’re in.
Get a Free Consultation. Our Experts Can Help You Figure Out What to Do Next.
- Book an online appointment: Get a free fertility consultation.
- CallW: 9311850412
- Email: info@fertilityworld.in
Is it safe to do multiple IVF cycles back to back?
Doctors often say that the body should have one menstrual cycle to heal between stimulations. Some women may be able to have back-to-back cycles, but this depends on how their hormones respond, how healthy their ovaries are, and how well they are recovering overall.
How many egg retrievals can a woman safely have?
There isn't a certain maximum number, but it's usually safe to do egg retrievals over and over again as long as they are watched carefully. Before suggesting another cycle, doctors look at the ovaries' reaction, hormone levels, and concerns such ovarian hyperstimulation.
Can too many IVF cycles damage the ovaries?
Current evidence indicates that IVF does not cause permanent damage to the ovaries when conducted under medical care. But stimulating the area over and over again could produce momentary pain, bloating, or hormonal imbalance.
What are the risks of repeated IVF cycles?
There are some physical concerns, including as ovarian hyperstimulation syndrome (OHSS), adverse effects from the injection, and small surgical risks from egg harvesting. It's also necessary to think about emotional stress, worry, and money problems.
How many IVF cycles are normal before pregnancy?
Many couples conceive within the first 3 cycles. However, cumulative success rates increase over multiple attempts. Doctors often reassess the treatment plan after 2–3 unsuccessful cycles.
How many IVF cycles are safe over age 40?
For women over 40, the number of safe cycles depends heavily on ovarian reserve and overall health. Because egg quality declines with age, doctors may recommend fewer attempts with own eggs before discussing donor egg options.
Does IVF become more successful after multiple cycles?
Doctors change how they provide medicine and study how the body reacts, which can make success better in later rounds. But the consequences are different for each age and illness.
How long should you wait between IVF cycles?
A lot of clinics say you should wait at least one full menstrual cycle before starting another round. This gives the body time to mend and hormones to return to normal.
When should you stop IVF treatment?
Doctors may suggest stopping when repeated cycles show poor ovarian response, declining egg quality, or significant health concerns. Emotional readiness and financial considerations also play a major role.